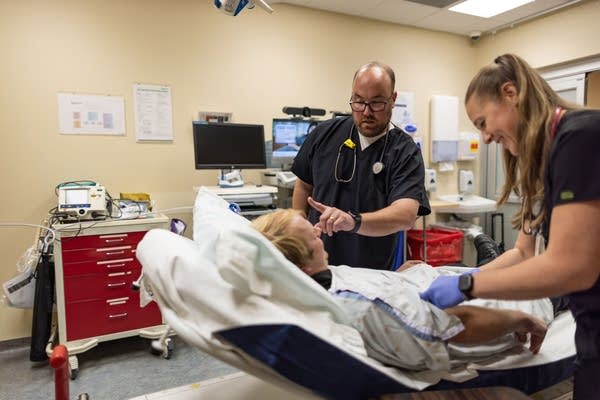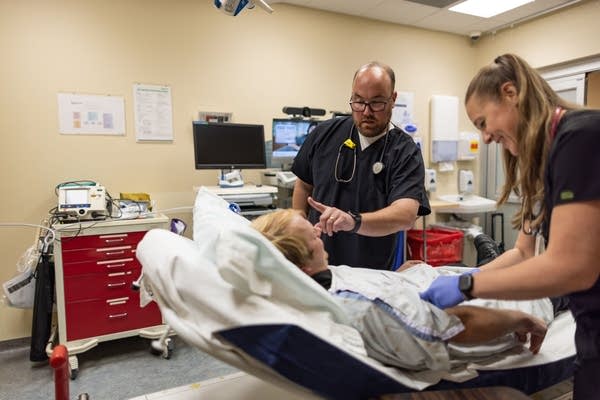
The University of Minnesota Medical School is adding a site to its rural family medicine residency program — the only program of its kind in Minnesota.
The medical school is partnering with Lakewood Health System to launch a residency in Staples, a small 3,000-person city in west-central Minnesota located across Todd and Wadena counties. Residents will begin with one year of training at North Memorial Health in Minneapolis, followed by two years in Staples.
Keri Bergeson, director of rural programs for the University of Minnesota Department of Family Medicine, explained that the aim of the program is to address the shortage of doctors in rural areas, with hopes that the residents plant roots and continue their careers in greater Minnesota.
“Right now, only 2 percent of residency training occurs outside of urban areas,” said Bergeson, who is a family physician herself.
“And then we sit here wondering why we don't have doctors in rural space — it’s because the vast majority of doctors stay where they train. They’ve got kids in the school, or a partner with a job, or they bought a house. If we don’t start training in other spaces, we're going to continue to face pretty significant workforce shortages.”

Staples will be the third rural family medicine residency program. The university’s medical school launched a program in Willmar last year, about an hour south of Staples, and just matched its first class of residents to its program in Grand Rapids in northern Minnesota this year. The Staples cohort is scheduled to start next summer.
Each of these three rural tracks is charged with training two resident physicians per year. The rural hospitals don’t have capacity to take on more trainees at this time.
“The rural track programs are super effective at training rural doctors, and they’re small,” Bergeson added. “So, they’re not the only solution to our rural workforce. They’re part of a bigger, strategic solution.”
The rural physician shortage is a nationwide issue, not unique to Minnesota. Exacerbating the need, rural areas tend to be marked by an aging population that typically requires more health care.
And the current stock of physicians in rural areas is closer to retirement age on average compared to urban areas. Bergeson said in Minnesota, one in four rural physicians plan to retire in the next five years.

While rural residency programs like these are new to the state, Bergeson said others across the country have been running for decades and have proven effective at bolstering the rural workforce.
“If you have any exposure to rural residency training, or you perform your residency training in a rural area, it’s five to six times more likely that you practice rural long term,” Bergeson said.
She believes the state of Minnesota could support an additional two to four rural family medicine residency programs in the future.
This is not the university’s only foray into rural physician training. For example, the University of Minnesota launched a medical campus in St. Cloud last year, which, while located in a larger city, is focused on educating physicians who aspire to work across greater Minnesota.
Students can start applying to the new program in Staples this September.